Analysis and Diagnosis of Laparoscopic Colectomy and Preoperative Oncology
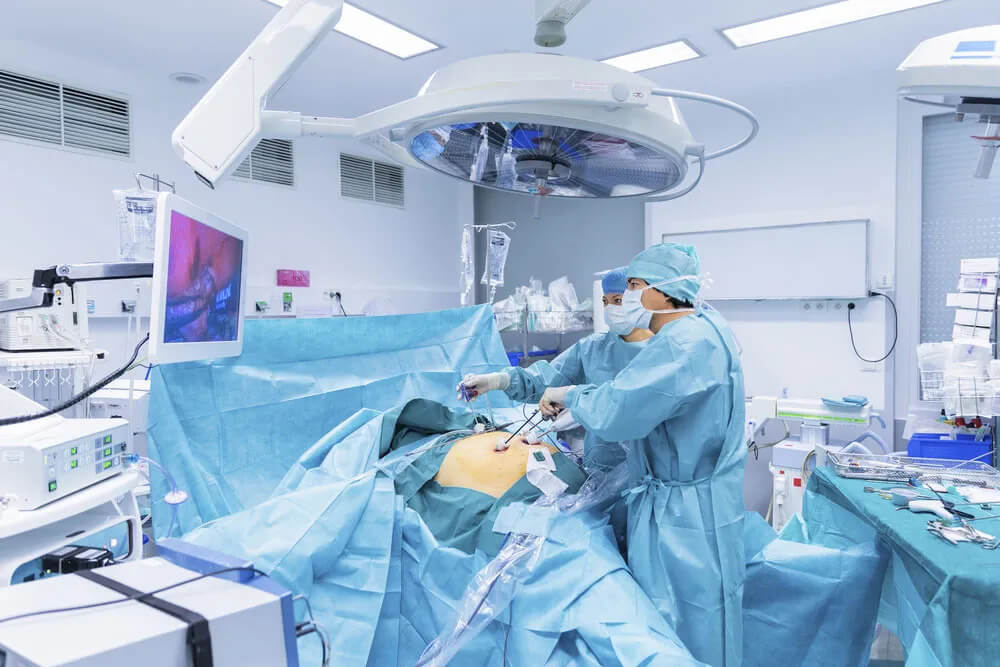
Table of Contents
Laparoscopic Surgery for Colon Cancer
Laparoscopic surgery is more expensive than open surgery because it takes longer and costs more equipment. Some costs cover shorter hospital stays. In the community, laparoscopic surgery is cheaper because patients can take care of themselves faster. Laparoscopic Trainer
For many reasons use of simulators is a workable choice like Laparoscopic Trainer.
Features Of Laparoscopic Surgery
Laparoscopic surgery was associated with less pain. Patients can eat faster than usual. There is faster expulsion You can return home faster than usual Principle of tumor treatment for laparoscopic surgery at the same level of open surgery. There was no difference between the groups in terms of the number of lymph nodes and the positive margin of surgery. Interlocal metastases are less common than wound metastases. Many people do not train in simulators such as laparoscopic trainers because of minimally invasive surgical techniques.
Laparoscopic Surgery Requirements
Laparoscopic cancer surgery requires a surgeon with experience in laparoscopic surgery and open surgery. Prolonged experience of laparoscopic surgery leads to less conversion. Patients should undergo a thorough physical examination before surgery to make sure the tumor is in the correct position. Adjacent tissue penetration and possible diffusion.
Study In the Oncology
The study publishes in the Oncology. They included patients with adenocarcinoma of the coecum, ascending colon, descending colon, and upper sigmoid colon. The patient had to be over 18 years old and give their informed consent. A total of 1248 patients randomizes.
Diagnosis
When certain exclusion criteria apply (including BMI> 30, benign conditions, other concomitant tumors), they leave with 536 patients in the laparoscopic group and 546 in the open group. The primary endpoint of the study was cancer-free survival 3 years after surgery. Secondary outcomes were short-term morbidity and mortality, number of positive resection grooves, local recurrence, port-site or wound recurrence, metastases, overall survival, and blood loss during surgery.
The open and the laparoscopic surgical protocol were almost identical. All surgical teams must have performed at least 20 laparoscopically assisted colectomies. Open surgery had to involve a surgeon who was a specialist in colon surgery.
Preoperative Imaging
The resects sends unfixed to a pathologist who measured tumor size, degree of tissue invasion, number of lymph nodes and TNM classification. Patients randomized to the laparoscopic group converts to the open group before surgery if it finds that the equipment was not working properly or that the right surgical team was not present. The results analyze according to the “intention-to-treat” principle. The use of preoperative imaging was not different between the groups. Laparoscopic Trainer
Duration Of the Laparoscopic Surgeries
This study shows that the operation time was longer in the laparoscopic group. However, they managed to reduce the duration of the laparoscopic surgeries as time went on, due to more trained staff, while they did not manage the same with the open surgeries (p = 0.027). Blood loss during laparoscopic colectomy was significantly lower than with open colectomy; 100 ml vs 175 ml (p <0.0001). Adherences were more frequently reported as a problem with laparoscopic than with open surgery (p = 0.02). 17% of the patients who initially places in the laparoscopic group converts to open surgery for various reasons. Laparoscopic Trainer.
Analysis Of Laparoscopic Colectomy
Postoperative microscopic examination showed that there were no differences between laparoscopically resected and open resected specimens. The groups also did not differ in terms of the number of positive resection grooves (p = 1.0) or the number of positive lymph nodes that harvests (median number 10 vs 10, p = 1.0).
After laparoscopic colectomy, patients tolerated an oral intake of 1 liter of fluid one day earlier than the open surgery (p <0.0001). Laparoscopic surgery was also associated with lower needs for opioid analgesics on day 2 (p <0.008) and 3 (p <0.0003) after surgery. Epidural uses less frequently in the laparoscopic group compared to the open group (p <0.02). Total morbidity was approximately the same after laparoscopic and open colectomy.
In total, there were complications in 21% in the laparoscopic group against 20% in the open group (p = 0.88). Reintervention requires in 7% in the laparoscopic group versus 5% in the open group (p = 0.13). 1% of patients in the laparoscopic group died, compared with 2% in the open group (p = 0.45). Postoperative hospitalization was 1 day shorter in the laparoscopic group than in the open; 8.2 vs 9.3 days (p <0.0001).
Conclusion
In summary, the COLOR study shows that even though the laparoscopic operation itself lasts longer than the open operation, the laparoscopically operated ones lose less blood intraoperatively. Tumors that resect laparoscopically did not differ tumors resected by open surgery, neither in stage, extent, size, histology, number of positive resection margins or number of positive lymph nodes.
After the operation, those who underwent laparoscopically operated fluid intake tolerated earlier, and that they had earlier bowel movements than those who operated openly. Laparoscopically operated patients also had less need for painkillers postoperatively. The group believes that it is not the operation time that is an important determinant in relation to postoperative pain, but that the tissue manipulation is the most important.
For more information visit our website: www.gerati.com